News
Archive for the ‘Pet of the Month’ Category
Pet of the Month – April 2017 – Diarmuid
by admin on April 1st, 2017
Category: Pet of the Month, Tags:
Distichiasis is a common condition in dogs. It occurs when eyelashes are abnormally positioned and emerge too close to the eyelid margin.
Distichiasis can occur in any breed of dog but is most commonly seen in the American Cocker and Cocker Spaniel, Miniature and Longhaired Dachshund, Bulldog and Weimeraner breeds.
What are the signs of distichiasis?
In many dogs the extra eyelashes do not cause a problem, but in some cases they can rub the surface of the eye and cause irritation. The most common signs that you will notice are increased blinking/squinting of the eye, increased watering, and redness of the ‘white’ of the eye.
What are the treatment options for distichiasis?
Distichiasis only requires treatment if the hairs are causing irritation, conjunctivitis or corneal ulceration. There are a number of treatment options:
- Ocular lubricants. In mild cases of distichiasis, daily use of a lubricating gel such as Viscotears, Geltears or Lacrilube may be sufficient to soften the hairs and reduce their irritation. Lifelong treatment will be required.
- Plucking. Sometimes the extra eyelashes can be plucked using special epilation forceps. This is particularly useful when there are only a few long hairs present. However, because the hairs will grow back after a few weeks, regular and lifelong treatment will be needed.
- Electrolysis. Under general anaesthesia, a fine electrode is inserted into each hair follicle and a current is applied to permanently destroy the hair follicle. Once the hair follicle is destroyed the distichia cannot regrow. However, because only those hairs that happen to be present at the time of treatment can be identified and removed, new hairs may emerge at a later date and also cause irritation. The success rate of electrolysis per treatment is around 70-80%. The procedure can be repeated a number of times if necessary. Rarely, electrolysis can cause some scarring and depigmentation of the eyelids, but this is not usually severe.
- Cryotherapy. This technique may be useful when many hairs are present. Under general anaesthesia, a probe is applied to the inner surface of the eyelid in the region of the hair follicles. Via this probe, the eyelid is frozen to destroy the hair follicles. The technique can cause some scarring and depigmentation of the eyelids. This procedure may also need to be repeated, and has a similar success rate to electolysis.
- Surgery. Excision of a very small portion of the eyelid margin from which the distichia are growing.
As the few distichia do not appear to be bothering Diarmuid’s eyes excessively, artificial tears are being used alone at present. Should the distichiasis become more of a problem then intervention along one of the lines described above will be necessary

Pet of the Month – March 2017 – Prince
by admin on March 1st, 2017
Category: Pet of the Month, Tags:
Our pet of the month this March is a delightful and photogenic Pomeranian puppy called Prince.
Prince had to have his right foot X-rayed after he jumped off a bed and landed awkwardly. Unfortunately, in the process he fractured all the toes of his right paw and was unable to bear weight on it.
Following surgery to stabilise the fractures using small metal pins we are really pleased to report Prince is making good progress and hopefully will be back to normal very soon.
Pet of the Month – February 2017 – Hadley
by admin on February 1st, 2017
Category: Pet of the Month, Tags:
Hadley has featured in this column before and his return to this newsletter is to highlight the need for vigilance in respect of skin tumours. Hadley suffers from a very serious form of skin cancer called a Mast Cell Tumour (MCT), and he is recovering very well following surgery to remove yet another recurrence. MCT can be very deceptive as they often start as small bumps which may remain static for many months before growing larger. It can be extremely difficult to contain, frequently recurs and may be life threatening.
MCT is the most common skin tumour in dogs; it can also affect other areas of the body, including the spleen, liver, gastrointestinal tract, and bone marrow. MCT represent a cancer of a type of blood cell normally involved in the body’s response to allergens and inflammation. Certain dogs are predisposed to MCT, including brachycephalic (flat-faced) breeds such as Boston Terriers, Boxers, Pugs, and Bulldogs, as well as retriever breeds, though any breed of dog can develop MCT.
When they occur on the skin, MCT varies widely in appearance. They can be a raised lump or bump on or just under the skin, and may be red, ulcerated, or swollen. In addition, many owners will report a waxing and waning size of the tumour, which can occur spontaneously or can be produced by agitation of the tumour, causing degranulation. Mast cells contain granules filled with substances which can be released into the bloodstream and potentially cause systemic problems, including stomach ulceration and bleeding, swelling and redness at and around the tumour site, and potentially life-threatening complications, such as a dangerous drop in blood pressure and a systemic inflammatory response leading to shock.
When MCT occur on the skin, they can occur anywhere on the body. The biological behaviour of these tumours can vary widely; some may be present for many months without growing much, while others can appear suddenly and grow very quickly. The most common sites of MCT spread (metastasis) are the lymph nodes, spleen and liver.
Diagnosis can be simply achieved via a fine needle aspirate. This requires no anesthesia and only rarely sedation. Early identification and surgical removal are key to the most favourable outcomes however aggressive forms may require radical surgery and necessitate referral to a specialist cancer referral centre.
Hadley initially found the operation sites to be very itchy after surgery, something not uncommon with MCT. After removing a few of his own sutures Hadley was given additional medication, resutured and had to wear a full body suit! We are pleased to report he is making very good progress.
Pet of the Month – January 2017 – Sophia
by admin on January 3rd, 2017
Category: Pet of the Month, Tags:
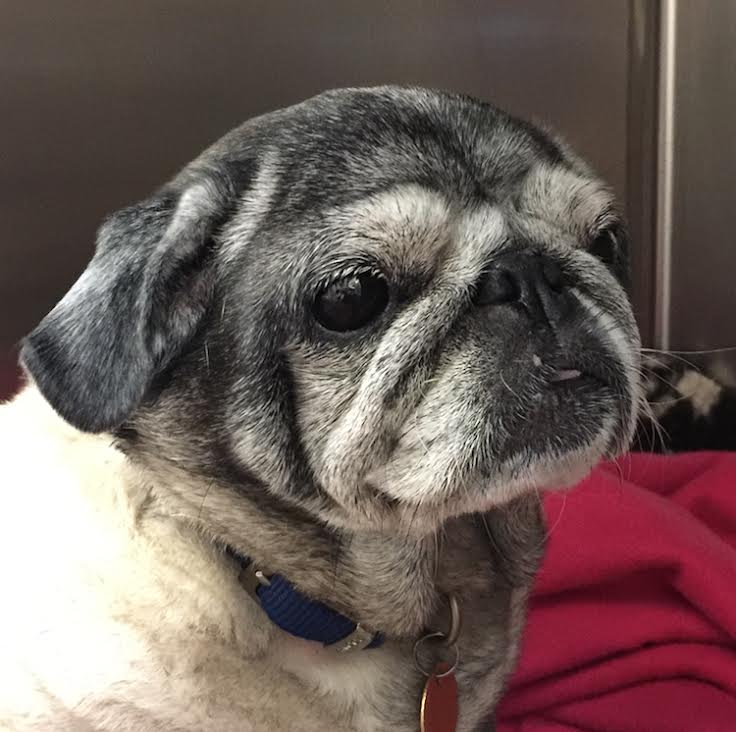 Pet of the month for January is Sophia, an 11-year-old Pug. She is seen here in post-op recovery having just had an ovariohysterectomy to treat a condition called pyometra.
Pet of the month for January is Sophia, an 11-year-old Pug. She is seen here in post-op recovery having just had an ovariohysterectomy to treat a condition called pyometra.
Pyometra is an infection of the uterus (womb). It is a common condition in older female dogs that have not been spayed but can occur in un-spayed dogs of any age. Occasionally we see cases occurring in cats.
What causes pyometra?
Each time a female dog has a season (usually about twice a year) she undergoes all the hormonal changes associated with pregnancy – whether she becomes pregnant or not. The changes in the uterus that occur during each season making infection more likely with age. A very common organism called E. coli, found in your dog’s faeces, usually causes the infection. We most commonly see cases of pyometra in the 4-6week period after a heat. Injections with some hormones to stop seasons or for the treatment of other conditions can also increase the risk of pyometra developing.
What are the signs of pyometra?
Pyometra is of course, only seen in females (since males do not have a uterus). It is more common in older females (above 6 years of age) but can be seen at any age. The signs usually develop around 6 weeks after the female has finished bleeding from her last season, but in some cases, the bitch appears to have a prolonged season.
Early signs that you may notice are that your dog is:
- Licking her back end more than normal
- Off colour
- Off her food
- Drinking more than normal (and will probably urinate more)
These signs will progress and you may see:
- Pus (yellow/red/brown discharge) from her vulva
- She may have a swollen abdomen
- Vomiting
- Collapse
If left untreated signs will worsen to the point of dehydration, collapse and death from septic shock.
Diagnosis
Your vet will probably suspect your dog has a pyometra based on your description of the signs and from their examination of your pet. They may suggest procedures such as ultrasound and blood tests confirm the diagnosis, rule out other possible causes and to check that your pet is well enough to undergo treatment.
Treatment
The treatment of choice for pyometra is surgery to remove the uterus as soon as possible. The operation is essentially the same as a routine spay, however, there is more risk involved and a higher chance of complications when the operation is being carried out on a sick pet. Your dog will also be given intravenous fluids (a drip), antibiotics and pain relief.
Most dogs will make a full recovery after treatment for a pyometra if the condition is caught early. Spaying your dog before she develops a pyometra will prevent this condition occurring.
We are delighted to report that Sophia has made a full recovery after surgery.
Pet of the Month – December 2016 – Smudgey
by admin on December 1st, 2016
Category: Pet of the Month, Tags:
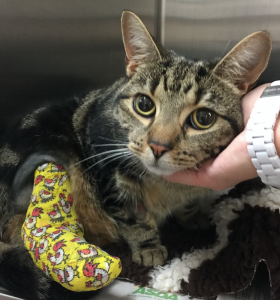
Smudgey is giving us a reproving look from the depths of a buster collar that should prevent him removing his indwelling urinary catheter.
 The catheter had to be placed under anaesthesia in an emergency procedure to relieve a potentially life-threatening condition called urethral obstruction.
The catheter had to be placed under anaesthesia in an emergency procedure to relieve a potentially life-threatening condition called urethral obstruction.
Urethral obstruction is a problem that occurs almost exclusively in male cats. This is because the urethra of a male cat is much longer and much narrower than that of a female cat, and so is more susceptible to becoming blocked.
Urethral blockage is not a common condition, but when it occurs it is painful, the cat will be unable to urinate despite repeated efforts, and it is a life-threatening emergency as it can cause acute kidney failure and death within 2-3 days if not managed appropriately
What are the signs of urethral obstruction?
A cat with urethral obstruction will usually show:
- Repeated attempts to urinate that are unproductive
- Crying or discomfort when straining to urinate
- Increased agitation, and there may be some vomiting
Depending on the underlying cause, you may also have noticed some other changes in your cat’s urinating behaviour over the preceding few days such as increased frequency of urination, straining, discomfort or even some blood in the urine.
Contact your vet immediately if you think your cat may have an obstructed urethra, as this is an emergency situation.
What causes urethral obstruction?
Several underlying conditions can cause obstruction of the narrow urethra of a male cat, including:
- A ‘plug’ in the urethra – this is usually an accumulation of proteins, cells, crystals and debris in the bladder that accumulates and lodges in the urethra
- A small stone (urolith) or an accumulation of very small stones – these form in the bladder but may become lodged in the urethra
- Swelling and spasm of the urethra – during inflammation of the bladder and urethra, whatever the cause, the inflammation may cause swelling of the wall of the urethra which may contribute to blockage, and in a number of cases the inflammation and irritation causes the muscle around the urethra (the urethral sphincter muscle) to go into spasm – this too can cause obstruction if the cat is not able to relax the muscle.
How is urethral blockage managed?
If your cat’s urethra is blocked, the vet will need to relieve the obstruction quickly.
Blood tests may be important to see if there are any significant complications. In particular, cats with a blocked urethra may develop acute kidney failure and may develop very high blood potassium concentrations; these are life-threatening complications that should be checked when possible.
X-rays or ultrasound may be needed to help determine the underlying cause of the obstruction and to help determine the best treatment method.
Under anaesthesia a catheter is passed into the urethra (via the penis) so that fluids can be infused to help flush out the obstruction (or sometimes to push it back into the bladder). These procedures have to be done very carefully to avoid damaging the delicate lining of the urethra.
If the obstruction is caused by spasm of the urethral muscle, simply sedating or anaesthetising the cat may be sufficient to allow easy passage of a catheter into the bladder.
What happens after the obstruction is relieved?
Once the obstruction has been relieved, the vet will want to infuse a sterile saline solution into the bladder via the catheter so that all the blood and debris (that will inevitably be present in the bladder) can be washed out. This is usually repeated several times to remove as much debris as possible to reduce the chance of re-obstruction.
Once this has been done, the vet will decide whether the urinary catheter can be removed. If there has been a severe blockage, your vet may want to leave a catheter in for a few days (usually no more than 2-3 days) to ensure urine can be produced while treatment is commenced for the underlying disease and inflammation.
What other treatments are given?
Further treatment depends on the underlying cause of the obstruction, the severity of the obstruction, and what (if any) complications have arisen. Any damage to the kidneys may be completely reversible, but cats will often have to receive intravenous fluids for several days if the kidneys have been affected. In addition to intravenous fluids, other drugs commonly used to help manage cats include:
- Other pain-killing (analgesic) drugs
- Drugs to help relieve spasm of the urethra (spasmolytics)
- Anti-inflammatory drugs to relieve the swelling in the urethra
Long-term management of the cat with urethral obstruction
In the short-term, while the initial swelling in the urethra settles down, cats may need to be on anti-inflammatory drugs, spasmolytics, and perhaps analgesics for several days and even up to a week or two.
Longer term, management is aimed at the underlying cause of the urethral obstruction. Cases associated with uroliths (stones in the urethra and bladder) will need to be managed with special diets to reduce the risk of their recurrence. Most cats with urethral spasm or urethral plugs are thought to have underlying feline idiopathic cystitis. These cats should be managed with painkillers and the aim of reducing stress.
If repeated episodes of obstruction occur despite appropriate management, in some cases a surgical operation can be performed (called perineal urethrostomy) to help open and widen the narrow end to the urethra. This should not be regarded as a first-line therapy though as it does not deal with the underlying cause, and the surgery can sometimes be associated with complications such as the risk of stricture formation and an increased risk of bacterial urinary tract infections.
Pet of the Month – November 2016 – Bruce
by admin on November 3rd, 2016
Category: Pet of the Month, Tags:
Poor Bruce! This is not the first time our practice cat has featured in this newsletter. At present Bruce is suffering from pancreatitis and is in our hospital.
Pancreatitis in cats has two forms, acute and chronic, which are usually diagnosed by symptoms and by ruling out other diseases. There are diagnostic tests for pancreatitis, but they are not always accurate, they can be costly, and can be quite invasive for a definitive diagnosis. Pancreatitis can also predispose your cat to other disease processes.
The pancreas is an organ that makes two primary products – digestive enzymes and insulin. Normally the digestive enzymes are released in an inactive form and are not activated until they reach the intestinal tract. This is to prevent the enzymes that are designed to break down food from coming into contact with the delicate pancreatic tissue.
In pancreatitis, for reasons yet unknown to us, these digestive enzymes will become activated while they are still in the pancreas. This results in significant inflammation and irritation to the pancreatic tissue, which can also cascade to other surrounding tissues such as the liver and intestinal tract. This can lead to secondary bacterial infections in the pancreas.
If the activation of the digestive enzymes is significant enough, then your cat can develop acute pancreatitis which can range from mild to severe and life threatening. If the activation of the digestive enzymes remains mild and continues long term, then your cat may develop chronic pancreatitis, which can result in the development of scar tissue in the pancreas, and eventually pancreatic insufficiency and predisposition to diabetes. It has been estimated that 30% or more of cats have chronic pancreatitis, but many may never show symptoms.
Acute pancreatitis:
Symptoms - Every cat will have different symptoms, some may have several, and some may have only one.
- Intense vomiting: Your cat may vomit multiple times over a period of hours or days, and may not be able to keep food down. This needs to be addressed quickly to prevent dehydration.
- Pain: Your cat may be sitting in a hunched position with their head tucked, or not want to be picked up or touched. Acute pancreatitis is very painful in all mammals.
- Anorexia:Your cat may be feeling intensely nauseous and painful, so it is unlikely that they will want to eat.
- Lethargy: Your cat may be extremely tired and lethargic.
- Diarrhoea: If your cat’s pancreas is so inflamed that it is not secreting digestive enzymes into the small intestine, then any food that your cat does eat may come out as diarrhoea with a very foul odour.
Diagnosis - With acute pancreatitis, we will need to begin treatment immediately. How we treat at this point will be based on the severity of the symptoms and blood sample results.
- Blood tests: As well as general haematology and biochemistry tests there are pancreas specific tests such as fPLI – this stands for feline pancreatic lipase immunoreactivity which can be elevated in pancreatitis in cats. However, while a positive test can confirm a diagnosis of pancreatitis, a negative test does NOT rule it out. It is possible to have a false positive with this test. The accuracy of this test has been estimated to be between 50-80%. So, while we may use this test to try and confirm a diagnosis of pancreatitis, we will not use it to make an initial diagnosis.
- Ultrasound: For an experienced ultrasonographer, this can be a good way to diagnose pancreatitis, by finding an enlarged, thickened pancreas on ultrasound. However, this requires a more advanced skill level of ultrasonagraphy than most general practitioners have.
- Biopsy: This is considered the gold standard for a 99.9% accurate diagnosis. However, this requires exploratory abdominal surgery which is invasive to your already sick cat, and it can take 2-3 days to get the histopathology results, so we do not do this routinely.
Treatment - The goal of treatment for acute pancreatitis is to reduce your cat’s pain and nausea, stabilize any electrolyte abnormalities, treat any secondary infections, and reduce the inflammation until your cat is able to heal.
- Pain management: This is one of the most important aspects of treating acute pancreatitis. Commonly used drugs are: Buprenorphine. This is a narcotic that has show to have excellent pain control in cats. This is our most common first line pain management for acute pancreatitis.
- Nausea: We have several anti-nausea medications that we will use in cats with acute pancreatitis. Most commonly used is Cerenia (maropitant). This is a fairly new drug that has quickly become our first line of defense for nausea in cats. This drug not only reduces nausea and vomiting, but it also has anti-inflammatory and anti-pain properties.
- Reducing gastric acid secretion in the stomach can help an already nauseated cat. We often use omeprazole.
- Antibiotics: We may use antibiotics to treat any secondary infections.
- Intravenous fluids: If your cat is having a hard time staying hydrated due to vomiting or not drinking, or if your cat has abnormal electrolytes, then we will start intravenous fluid therapy.
- Syringe feeding: If is very important that you cat eats. If they are too nauseous to eat, we may syringe feed them a very bland diet or a prescription diet.
Possible long term effects: Acute pancreatitis can lead to destruction of a fair amount of pancreatic tissue. How much tissue is affected can determine what happens next. Some of the more common sequelae are:
- Scar tissue: After the inflammation subsides, there is a chance of scar tissue developing in the healing process. As long as there is enough healthy tissue remaining, then your cat may never have any additional problems.
- Chronic pancreatitis: This is what happens when your cat’s pancreas continues to have low grade chronic inflammation. This can result in regular vomiting and anorexia episodes.
- Pancreatic insufficiency: When too much of your cat’s pancreas that makes digestive enzymes is destroyed, either by severe acute pancreatitis, or by chronic pancreatitis, eventually the pancreas will not be able to make enough enzymes to digest food. Your cat may then have large fluffy diarrhea and an increase in vomiting. This can be treated by giving your cat synthetic digestive enzymes.
- Type I diabetes: When enough of your cat’s pancreas that makes insulin is destroyed, it will not be able to make enough insulin to counteract the glucose in the body. Your cat may then develop diabetes and will need to be started on insulin injections.
Chronic pancreatitis:
The symptoms of chronic pancreatitis are very similar to acute pancreatitis, but on a milder scale. A common pattern we will hear is that your cat will vomit several times a day for a few days, not want to eat, and may act uncomfortable and lethargic, and then a few days later, will be fine until the next episode. These symptoms can also be similar to inflammatory bowel disease, so we may ask you lots of questions about exactly what goes on with each episode, and frequency to try and distinguish between the two.
Diagnosis again is similar to acute pancreatitis, but it can be harder as the blood work will be more likely to look normal, fPLI will only be positive if there is significant inflammation, and ultrasound will be even harder to detect. There is a blood test available that will test for two pancreatic enzymes and two intestinal enzymes to try and differentiate between pancreatitis and inflammatory bowel disease, but if it is negative, it still doesn’t rule either one out for sure.
Treatment most commonly is symptomatic, with pain medications, antibiotics, and anti-nausea medications. For cats who do have routine flare ups of chronic pancreatitis, we may want to treat long term with Cerenia as a preventative. We have a few other preventative treatment options as well if Cerenia is not an option.
While pancreatitis is one of the more painful and potentially nauseating diseases we can see in cats, as you have just read above there are things we can do to decrease its effects and help your cat to feel better.
Pet of the Month – October 2016 – Margot
by admin on October 7th, 2016
Category: Pet of the Month, Tags:
Margot is currently doing really well, recovering from an operation to correct “cherry eye’.
Cherry eye, or prolapse of the gland of the third eyelid, is quite common in small dogs and refers to a pink mass protruding from the animal’s eyelid;. The prolapsed gland itself rarely causes discomfort or damage to the eye, so the repair is mostly cosmetic. Most people choose to repair it, because it can have a very unpleasant appearance.
The gland contributes about 40% of the total tear-production of the eye and it is therefore imperative to aim to preserve the gland if possible as removal can cause a dry eye which can lead to damaged vision. If this does happen, it is controllable with medications, but it is preferable to prevent it. The most common surgical approach is a technique in which the gland is re-positioned using a mucosal pocket, creating a new envelope for the gland to sit within, but taking care to leave a few millimetres on either side to allow tears to drain freely. The unaffected side is often operated on pre-emptively.
Pet of the Month – September 2016 – Daisy
by admin on September 1st, 2016
Category: Pet of the Month, Tags:
When young Daisy returned from her travels with a wounded and unstable right hock joint her owner brought her to the surgery straight away. Radiographs revealed the hock joint to be extremely unstable which necessitated a referral to an orthopaedic specialist.
Daisy’s hock was stabilised with an external fixator and bandaged. External fixation consists of inserting two or more pins each in undamaged areas of the bones proximal and distal to the fracture site. The pins are connected by clamps or putty to keep them rigid.
Undaunted by her escapade Daisy managed to escape from an open window on her first night home from the specialist. After a half hour chase she was caught and returned to what had been thought to be a secure enclosure, now with even tighter security. Her hock had to be re-radiographed the next day to check that no damage had been incurred and we are pleased to report that she is making very good progress.
Pet of the Month – August 2016 – Brambie
by admin on August 1st, 2016
Category: Pet of the Month, Tags:
Brambie first visited the practice as a second opinion for recurrent bladder/urination problems. A scan revealed she had bladder stones which had not been picked up by her previous vet.
We surgically removed her bladder stones and are delighted to report that she is doing very well.
For your interest we include further information on bladder stones below.
What are the symptoms of struvite bladder stones?
The symptoms of bladder stones are very similar to the symptoms of an uncomplicated bladder infection or cystitis. The most common signs that a dog has bladder stones are hematuria (blood in the urine) and dysuria (straining to urinate). Hematuria occurs because the stones rub against the bladder wall, irritating and damaging the tissue and causing bleeding. Dysuria may result from inflammation and swelling of the bladder walls or the urethra, from muscle spasms, or due to a physical obstruction to urine flow caused by the presence of the stones. Veterinarians assume that the condition is painful, because people with bladder stones experience pain, and because many clients remark about how much better and more active their dog becomes following surgical removal of bladder stones.
Large stones may act almost like a valve or stopcock, causing an intermittent or partial obstruction at the neck of the bladder, the point where the bladder attaches to the urethra. Small stones may flow with the urine into the urethra where they can become lodged and cause an obstruction. If an obstruction occurs, the bladder cannot be emptied fully; if the obstruction is complete, the dog will be unable to urinate at all. If the obstruction is not relieved, the bladder may rupture. A complete obstruction is potentially life threatening and requires immediate emergency treatment.
My dog has struvite bladder stones. What does that mean?
Dogs, like people, can develop a variety of bladder and kidney stones. Bladder stones (uroliths or cystic calculi), are rock-like formations of minerals that form in the urinary bladder, and are more common than kidney stones in dogs. One of the more common urolith in the dog is composed of magnesium ammonium phosphate hexahydrate. The more common name for this type of bladder stone is “struvite bladder stone”.
How did my dog get them?
Normal dog urine is slightly acidic and contains waste products from metabolism including dissolved mineral salts and other compounds. Struvite is a normal component of dog’s urine and will remain dissolved as long as the urine is acidic and is not too concentrated. If the urine becomes exceptionally concentrated or if it becomes alkaline, struvite crystals will precipitate or fall out of solution.
In dogs, struvite bladder stones usually form as a complication of a bladder infection caused by bacteria that produce an enzyme known as urease. This enzyme breaks down the urea that is normally present in the urine causing an excess production of ammonia; this ammonia production then causes the urine to become alkaline. Ammonia in the urine also causes bladder inflammation. Under these environmental conditions, struvite crystals will precipitate out of solution and collect around any cells or debris that may have formed in the bladder as a result of inflammation. Female dogs tend to get these types of bladder infections and stones much more frequently than males, probably because their shorter, wider urethra makes it easier for bacteria to pass up the urethra into the bladder. In some studies, up to 85% of dogs with struvite bladder stones were female.
Other causes of alkaline urine such as certain kidney diseases, long-term use of diuretic drugs or antacids, and other conditions that cause elevated urine pH or elevated levels of urinary phosphorus or ammonia can also predispose a dog to the formation of struvite bladder stones.
How common are struvite bladder stones?
Bladder stones are somewhat common in dogs, and struvite stones are the most common; in clinical studies, up to 26% of all bladder stones were found to contain struvite. Together, struvite and calcium oxalate uroliths have been found to comprise over 85% of all uroliths submitted for laboratory analysis in a recent study. Based on the results of tens of thousands of stone analyses, it has been found that the number of struvite bladder stones has been declining in dogs while the number of calcium oxalate stones has been increasing during the past ten years. Struvite uroliths were noted to be more common in female dogs and calcium oxalate uroliths in male dogs. Breeds most commonly diagnosed with struvite and calcium oxalate bladder stones included: shih tzu, miniature schnauzer, bichon frisé, lhasa apso, and Yorkshire terrier.
How are struvite bladder stones diagnosed?
In some cases, your veterinarian may be able to palpate (feel) struvite stones in the bladder if the dog is relaxed and the bladder isn’t too painful. However, some stones are too small to be felt this way. Often, bladder stones are diagnosed by means of an x-ray of the bladder, or by means of an ultrasound. Struvite stones are almost always ‘radiodense’, meaning that they can be seen on a plain radiograph. However, sometimes bones or other overlying body parts will interfere with the ability to see bladder stones with regular x-rays, in which case your veterinarian may recommend a contrast study, a specialized technique that uses dye to outline the stones in the bladder, or a bladder ultrasound.
These imaging procedures will identify the presence of a bladder stone, but will not definitively tell your veterinarian the composition of the stone. The only way to be sure that a bladder stone is made of struvite is to have the stone analyzed at a veterinary laboratory.
In some cases, your veterinarian may make an educated guess about the type of stone that is present, based on the radiographic appearance and results of a urinalysis. For example, if x-rays show that there are one or more stones present in the bladder, and the results of the urinalysis show the presence of alkaline urine along with numerous struvite crystals, your veterinarian may make a presumptive diagnosis of struvite bladder stones and recommend treatment accordingly.
How are struvite bladder stones treated?
There are three primary treatment strategies for struvite bladder stones:
1) Feeding a special diet to dissolve the stone(s)
2) Non-surgical removal by urohydropropulsion
3) Surgical removal
1) Feeding a special diet: The use of special therapeutic diets to dissolve struvite bladder stones is often recommended in cases where the risk of a urinary tract obstruction is relatively low. These diets typically are restricted in protein, phosphorus and magnesium and are formulated to promote formation of acidic urine (with a pH less than 6.5). This formulation helps dissolve struvite stones that are already present in the urine, and prevents formation of further stones. Dissolution of the stones is further enhanced by increased water intake, which will serve to dilute the urine.
Since most dogs with struvite bladder stones developed them as a result of a bladder infection, the dog will also be placed on antibiotic therapy while the stones are being dissolved. This is important because, as the layers of stone are dissolved, bacteria that have become trapped in the layers of stone are released into the bladder; if left untreated these bacteria can set up another infection. Some dogs may experience dissolution of struvite stones within two weeks while others may take up to 12 weeks. Your dog will need to have antibiotics during this entire period of time. If your dog is placed on dietary therapy to dissolve the bladder stones, your veterinarian will recommend that a urinalysis and bladder x-rays should be performed approximately every four to six weeks during treatment.
Some bladder stones can be ‘mixed’ or composed of multiple layers of different types of mineral, which may complicate treatment. If follow-up x-rays show that the stones are no longer dissolving, this may indicate that the stones are mixed, and the treatment plan may need to be adjusted.
2) Non-surgical removal: If the bladder stones are very small it may be possible to pass a special catheter into the bladder and then flush the stones out, in a technique called urohydropropulsion. In some cases, this procedure may be performed with the dog under heavy sedation, although general anesthesia is often necessary. If your veterinarian has a cystoscope, small stones in the bladder or urethra can sometimes be removed with this instrument, thus avoiding the need to cut the abdomen and bladder open. Either of these procedures may also be used to obtain a sample stone for analysis so that your veterinarian can determine if dietary dissolution is feasible.
3) Surgical removal: Surgery is indicated in dogs that have a large number of stones in their bladder, if there is an increased risk that the patient will develop an obstruction in the urinary tract, or if the client wishes to have the problem resolved as quickly as possible. Male dogs are at a much higher risk of developing an obstruction in the urinary tract as a result of bladder stones, so when bladder stones are diagnosed in a male dog, your veterinarian will often strongly recommend surgical removal. Surgery is also indicated if dietary treatment was not successful in eliminating the stones, or If it appears that the stones are composed of a mixture of mineral types. Your veterinarian will discuss the appropriate treatment strategy for your dog, based on your individual situation.
Are there any other treatment options?
In some selected referral centers, another option may be available to treat bladder stones. This option is ultrasonic dissolution, a technique in which high frequency ultrasound waves are used to disrupt or break the stones into tiny particles that can then be flushed out of the bladder. It has the advantage of immediate removal of the offending stones without the need for surgery. Your veterinarian will discuss this treatment option with you if it is available in your area.
How can I prevent my dog from developing struvite bladder stones in the future?
Dogs that have experienced struvite bladder stones will often be fed a therapeutic diet for life. Diets lower in protein, phosphorus and magnesium and promote acidic urine are recommended. The preventative diet is NOT the same as the diet that promotes dissolution of the stones. In certain cases, medications to acidify the urine may be required. In addition, careful routine monitoring of the urine to detect any signs of bacterial infection is also recommended. Bladder x-rays and urinalysis will be performed one month after successful treatment, dietary or surgical, and then every three to six months for life. Dogs displaying any clinical signs of urinary tract infections such as frequent urination, urinating in unusual places, painful urination or the presence of blood in the urine should be evaluated immediately. Keep in mind that the greatest risk factor for developing struvite bladder stones in the dog is a urinary tract infection.
Pet of the Month – July 2016 – Hedgie!
by admin on July 1st, 2016
Category: Pet of the Month, Tags: Tags: hedgehog, pet

This week’s Pet of the Month is a small hedgehog we have chosen to highlight the fantastic work our vets and nurses do treating wildlife. A few years ago we were very fortunate to have a Wildlife Unit built in our garden funded by The Body Shop and WADARS Animal Rescue. This small hedgehog was brought in to us injured, by a member of the public. We checked him over thoroughly under anaesthetic and cleaned up his wounded leg. He is now starting to eat and recover. We hope he will be moving on to a hedgehog rehabilitation centre shortly and in due course ‘Hedgie’ should be able to return to the countryside.